There is no such thing as a bad exercise, medication or asana, but there is such a thing as a badly prescribed exercise, medication or asana. I hear it all the time: cross fit is bad for you, yoga is bad for you, pilates is bad for you, XYZ medication is bad for you. Firstly, medicine was always designed to help us short term and was not intended for long term use. When the body is not in synchronisation, or there has been some sort of injury or trauma, medication will always help. However, it’s then the responsibility of the patient to do their best to restore the body to optimal homeostasis so that it can recover and fight off what ever comes next. All pain is multifactorial and one issue cannot be fixed with one thing. For example if you have a headache, does this mean you are short of an aspirin? We may take an aspirin short term to help, but we really need to look at the root cause rather than chasing symptoms. Secondly, recurring influenza that we seem to see ever winter, does this mean we are short of a vaccine for every flu strain? It’s the fish bowel analogy – either “Germ Theory: “Isolate the fish and give it a vaccination”, or “Terrain Theory: we must clean the tank.” I’ll leave you to ponder these thoughts!

The parent child relationship is predominate in any sort of medicine, healthcare system or therapy. The transactional model is used: this is where the person giving the treatment plays the parent and we end up playing the child. I always ask clients to consider investigating how to think, rather than being told what to think. We all have the three persona characters in us which are parent, child and adult. The ideal situation is that we start to engage in adult to adult relationships and stop behaving as the child archetype, relying on others for the answers or to fix us. “If you choose to alter your dependency cycle the choice is yours and therefore the power becomes yours” Emma Lane. This is so important at a time of social media and press bombarding, doing your own research on any topic from authorised sources will always be a slightly different answer to what you are actually hearing/being told. Having the ability to look at both sides of the three sides of the coin is essential.
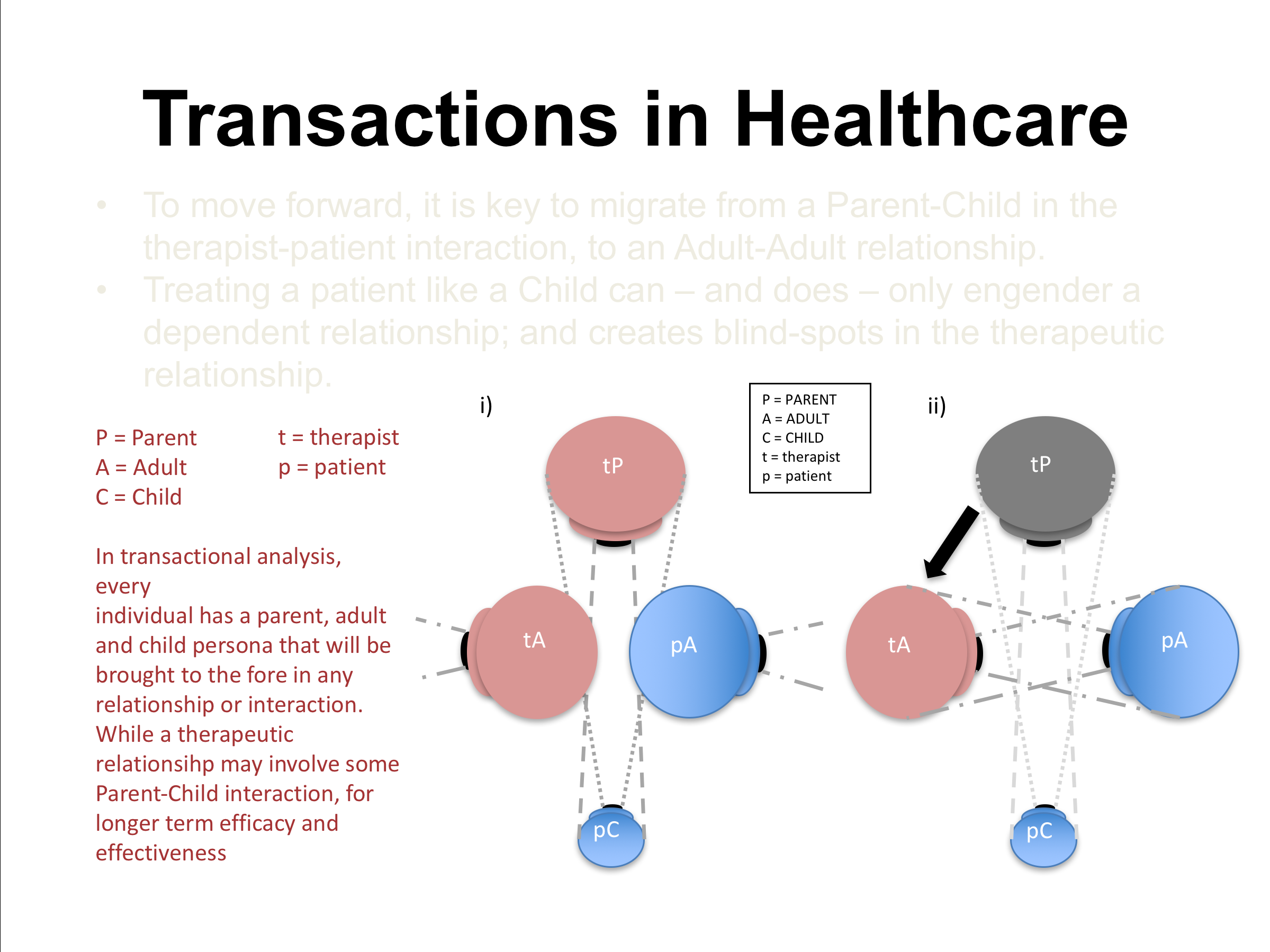
Matt Wallden slide
Movement matters
I have many colleagues who are yoga teachers who will not teach certain asanas as they say they are dangerous. This I have heard for all sorts of movement forms from the London marathon, to ballet, to cross fit and pilates. Well firstly there is no such thing as a bad exercise or asana, but there is such a thing as a badly prescribed exercise, asana or movement. One size does not fit all; we are all as different on the outside as we are on the inside. Ask any surgeon or gynaecologist.
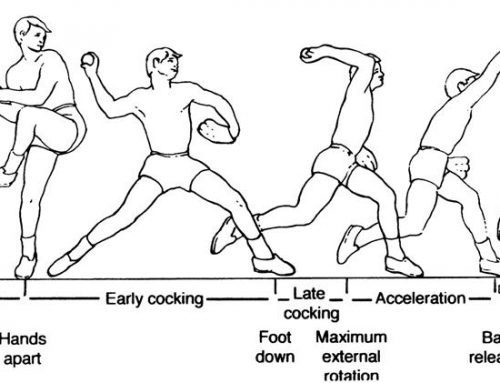
When we do any sort of movement, we do what is called force generation and it’s in order to deal with the task in hand and very dependent on environmental demands. Research tells us that TVA should fire first, meaning the tonic motor-neurons should fire ahead. So for example the bowler in cricket would be generating force from the ground upwards to be expressed out through the upper extremity and hand. Therefore the force generation sequence is:
Lower extremity- pelvis- torso-shoulder girdle- upper extremity and hand. The force generation reversed would be, for example, a diver entering the water from a diving board.
So why do some of us hate some exercises or asanas and why do they do us more harm than good?
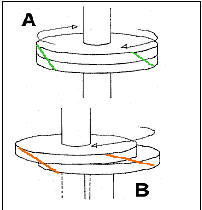
Not everyones’ bones, body type, posture, flexibility, strength threshold (plus so many other factors) are best designed for this movement or asana. For example, look at the cog wheel below. In Diagram A, joints are not only in alignment but are probably shaped correctly and under the right stresses and torque. Diagram B shows that for whatever reason, the joints are not in alignment. This can be anything from Beighton scale flexibility, load, central nervous system and surrounding structures. If this person does any form of repetitive movement which is not right for that body at that stage – such as golf swing, a cross fit exercise, ballet exercise, or a yoga asana – that person will incur more discomfort, injury or otherwise worsen the situation without getting the whole body as optimal as possible, including the joints to neutral.
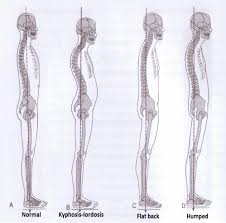
Look at the diagram below of the postures. I’m mainly looking at the bones. You will need more energy and have a faulty recruitment patterns if you are not at neutral. A 2013 research paper- Adverse Events Associated with Yoga: A Systematic Review of Published Case Reports and Case Series stated on yoga asana: “As yoga has been shown to be beneficial for a variety of conditions [65], [66], [68], it can also be recommended to patients with physical or mental ailments, as long as it is appropriately adapted to their needs and abilities and performed under the guidance of an experienced and medically trained yoga teacher. Especially, patients with glaucoma should avoid inversions and patients with compromised bone and other musculoskeletal disorders should avoid forceful or competitive yoga forms. Yoga should not be practiced while under the influence of psychoactive drugs. As any other physical or mental practice, yoga is not without risk. However, given the large number of practitioners worldwide [6]–[8], only relatively few serious adverse events have been reported in healthy individuals. Therefore, there is no need to discourage yoga practice for healthy people. “Holger Cramer, 1 , * Carol Krucoff, 2 and Gustav Dobos 1
A 2018 research paper titled: A 4-year Analysis of the Incidence of Injuries Among CrossFit-Trained Participants, in the Orthopaedic Journal of Sport Medicine stated that “Our findings suggest that CrossFit training is relatively safe compared with more traditional training modalities. However, it seems that those within their first year of training as well as those who engage in this training modality less than 3 days per week and/or participate in less than 3 workouts per week are at a greater risk for injuries”.Yuri Feito, PhD, MPH,*† Evanette K. Burrows, MPH,‡ and Loni Philip Tabb, PhD‡
And finally of course, it goes back to our own personal experience and perception – our conditioning as Osho calls it. A 2015 research paper:“The Biological Effects of Childhood Trauma states that “In a longitudinal study of individuals who had experienced abuse and neglect during childhood, only 22% of those who had been abused or neglected achieved resiliency based on a comprehensive assessment of healthy adult functioning, by the time they reached young adulthood [264]. Females who grew up in poverty and were not maltreated were more likely to show resilience [264]. While we have some important evidenced-based treatments for child victims, it is in our interest to put in place a national infrastructure of primary child trauma prevention as the less costly option for future victims and for society. Understanding the neurobiological consequences of child trauma will assist in treating child and adult victims, who tend to be more treatment refractory and may have a different endophenotype, than individuals with medical (including mental health) disorders who do not have such histories. Nevertheless, more work is needed to understand the neurobiological consequences of chronic stress on a child’s developing brain and body so that we can treat the adverse medical and mental health outcomes of early life stress in those cases (e.g., warfare, natural disasters, child maltreatment) where prevention and effective early intervention may not occur. Such understanding of the neurobiology and genetic influences of child trauma on child development will lead to novel and effective approaches to treatments (e.g., personalized medicine)”. Michael D. De Bellis, MD, MPH and Abigail Zisk A.B.
Bibliography
Matt Wallden – Covid 19
Emma Lane – Integrated health
A 4-Year Analysis of the Incidence of Injuries Among CrossFit-Trained Participants. Published online 2018 Oct 24. doi: 10.1177/2325967118803100
Adverse Events Associated with Yoga: A Systematic Review of Published Case Reports and Case Series. Published online 2013 Oct 16. doi: 10.1371/journal.pone.0075515
“Holger Cramer, 1 , * Carol Krucoff, 2 and Gustav Dobos 1
“The Biological Effects of Childhood Trauma”. Published online 2014 Feb 16. doi: 10.1016/j.chc.2014.01.002
Michael D. De Bellis, MD, MPH and Abigail Zisk A.B.